This article is just for the ladies.
Guys, go here instead. Thanks.
I’ve actually held off on posting this, because I wonder if I don’t divulge too much on this website sometimes.
As a rule, I prefer to write about things that I’ve personally experienced — with the hope that it will help someone else in some small way.
My theory is: If I wondered about how something works or how something’s done, then chances are someone else has wondered the same things.
That is what fuels my desire to keep writing these sometimes overly-personal stories… like today’s.
After a friend of mine told me that she was experiencing something similar and asked if I had any tips, suggestions, or little-known facts that she might need to know, that was all the motivation I needed to share my experience of having a laparoscopy to remove cysts from my ovaries — caused by severe endometriosis.
I have affectionately subtitled today’s post:
“How I Bid A Fond Farewell To My Baseball and My Golf Ball”
Yep, today’s post is a firsthand account of a medical procedure that I had done.
And since I have absolutely no modesty (or would that be no common sense???) I’ve even included some very non-flattering photos of myself in the height of my pre- and post-surgery delirium. (You can click on each my laparoscopy endometriosis pictures to view the full-size images.)
So… here we go!
Endometriosis & Ovarian Cysts
Ladies: Have you got endometriosis and/or cysts on your ovaries?
If so, then there’s probably a laparoscopy in your future.
I’m here to tell you it’s not that bad.
I had severe endometriosis and 2 ovarian cysts.
The one on the left ovary was initially measured at 4.67 cm. The one on the right ovary was 3.5 cm — that’s larger than the ovaries themselves. After my endometriosis surgery, the doctor said that the cysts were actually much larger than the ultrasound had measured, and one (the “baseball”) was even larger than my uterus! My doctor found it hard to believe that I never had any worse symptoms because these cysts were so large.
For what it’s worth, ovarian cysts are fairly common.
Laparoscopic surgery (often referred to as “lap surgery”) is the only real way to diagnose endometriosis. Your gynecologist or even family doctor may have made an assumptive diagnoses based on your symptoms, but a true diagnoses can only be made when the endometrial adhesions are seen. The description of the surgery (-scopic) suggests that the doctor intends to merely look and see if adhesions are present, but once adhesions are found they are removed during the same procedure. Endometrial adhesions are most frequently found on the ovaries and fallopian tubes, but may be present anywhere in the abdomen. Endometriosis on the ovaries can form cysts, called endometrioma. Source
Forms Of Endometriosis Treatment
 Instead of a laparoscopy, I could have tried a more passive endometriosis treatment (like hormone therapy which puts your body into full menopause temporarily, or 1 shot for 3 months to shrink up the cysts) — but I chose the most aggressive form of treatment.
Instead of a laparoscopy, I could have tried a more passive endometriosis treatment (like hormone therapy which puts your body into full menopause temporarily, or 1 shot for 3 months to shrink up the cysts) — but I chose the most aggressive form of treatment.
Actually, I tried birth control pills for a month to see if they would shrink the cysts at all (as they typically do when it’s endometriosis).
But my cysts didn’t shrink at all. Instead, both got significantly larger — which meant they could have been cancerous. The only way to know for sure was to remove them. So I did.
Here’s what it’s like to have laparoscopic surgery for endometriosis, or at least the way things went for me…
The Things They Tell You About (…with a few notes added by me)

![]() You have to drink 1 full bottle of Magnesium Citrate the day before your endometriosis surgery. (It’s not nearly as bad-tasting as I thought it would be! Jim even tried it & agreed. It’s kinda like Mountain Dew… but not.)
You have to drink 1 full bottle of Magnesium Citrate the day before your endometriosis surgery. (It’s not nearly as bad-tasting as I thought it would be! Jim even tried it & agreed. It’s kinda like Mountain Dew… but not.)
![]() After midnight the night before your surgery, you can’t use tobacco products, breath mints, or gum. Nor should you take any of your “regular” medicines the day of surgery — unless instructed by your doctor.
After midnight the night before your surgery, you can’t use tobacco products, breath mints, or gum. Nor should you take any of your “regular” medicines the day of surgery — unless instructed by your doctor.

![]() You can’t wear nail polish, hand lotion, hairspray, deodorant, or makeup on the day of your surgery. (Not exactly true. I told the nurse I’d forgotten that part & had all of the above on. She said it was okay.)
You can’t wear nail polish, hand lotion, hairspray, deodorant, or makeup on the day of your surgery. (Not exactly true. I told the nurse I’d forgotten that part & had all of the above on. She said it was okay.)
![]()
 You have to arrive at the hospital an hour-and-a-half before your scheduled surgery time. (This was for all of the time it took to fill out simple paperwork …get changed into your cap & gown and …get prepped for surgery.)
You have to arrive at the hospital an hour-and-a-half before your scheduled surgery time. (This was for all of the time it took to fill out simple paperwork …get changed into your cap & gown and …get prepped for surgery.)
![]() You should wear really comfortable clothing to surgery. (I think everyone who was scheduled for outpatient surgery that morning wore the same 2-piece jogging suit that I’d recently purchased at Kohl’s!)
You should wear really comfortable clothing to surgery. (I think everyone who was scheduled for outpatient surgery that morning wore the same 2-piece jogging suit that I’d recently purchased at Kohl’s!)
![]() Be sure that you have your driver’s license and your health insurance card the day of your surgery.
Be sure that you have your driver’s license and your health insurance card the day of your surgery.

![]() They insert an IV into the top of your hand moments after you walk into the pre-surgery room. (Which, for me, was a good thing because that’s the part I had feared the most — I don’t like needles.)
They insert an IV into the top of your hand moments after you walk into the pre-surgery room. (Which, for me, was a good thing because that’s the part I had feared the most — I don’t like needles.)
![]() They give you 2 or 3 pills to take soon after you arrive. Supposedly, these help prevent nausea after the anesthesia and lessen any anxiety prior to being rolled in for surgery. They must’ve worked — because I didn’t have any nausea or anxiety right before or right after surgery.
They give you 2 or 3 pills to take soon after you arrive. Supposedly, these help prevent nausea after the anesthesia and lessen any anxiety prior to being rolled in for surgery. They must’ve worked — because I didn’t have any nausea or anxiety right before or right after surgery.
![]() Overall, my endometriosis surgery took an hour and a half. I had an additional endometrial ablation. (It was an “option”, so I went for it. Geesh, even at the gyno, they’re trying to upsell ya!) UPDATE: I am SO incredibly glad I had the ablation. Here is it 9 years later, and no periods for those 9 years has been absolutely amazing!
Overall, my endometriosis surgery took an hour and a half. I had an additional endometrial ablation. (It was an “option”, so I went for it. Geesh, even at the gyno, they’re trying to upsell ya!) UPDATE: I am SO incredibly glad I had the ablation. Here is it 9 years later, and no periods for those 9 years has been absolutely amazing!
![]() They access your pain after surgery on a scale of 1 to 10 during your time in recovery. (Not true. In my case they said, ‘How do you feel?’ and ‘What hurts most?’ My answers to those alone determined 1 Percocet or 2.)
They access your pain after surgery on a scale of 1 to 10 during your time in recovery. (Not true. In my case they said, ‘How do you feel?’ and ‘What hurts most?’ My answers to those alone determined 1 Percocet or 2.)
![]() Once you can hold down food & drink, and urinate… you will be discharged from outpatient surgery. (They actually never tested my ability to urinate.)
Once you can hold down food & drink, and urinate… you will be discharged from outpatient surgery. (They actually never tested my ability to urinate.)
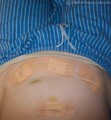
![]() Your belly will be puffy for several days following endometriosis surgery — due to the fact that they super-extend the stomach with a bunch of air in order to give the doctors enough room to work. (This was very weird. Thankfully, today’s lower, hip-hugging fashions helped to accommodate for the extra inch or so of space that my stomach now required. My belly actually got even more bloated as the days went on — probably due to the fact that I wasn’t able to have a B.M. for 4 days. I’ve since learned that’s a side effect of the Percocet.)
Your belly will be puffy for several days following endometriosis surgery — due to the fact that they super-extend the stomach with a bunch of air in order to give the doctors enough room to work. (This was very weird. Thankfully, today’s lower, hip-hugging fashions helped to accommodate for the extra inch or so of space that my stomach now required. My belly actually got even more bloated as the days went on — probably due to the fact that I wasn’t able to have a B.M. for 4 days. I’ve since learned that’s a side effect of the Percocet.)
![]()
 You will be able to go back to work after 24 hours. (Cough, cough, yea right! There was NO way I could stand fully erect, let alone get my mind off the pain & swelling — for at least 2 days. But I actually needed 3 days off work due to the added swelling & pain in my belly — see below.)
You will be able to go back to work after 24 hours. (Cough, cough, yea right! There was NO way I could stand fully erect, let alone get my mind off the pain & swelling — for at least 2 days. But I actually needed 3 days off work due to the added swelling & pain in my belly — see below.)
![]() The carbon dioxide that remains in your body after the surgery may present itself as shoulder pain or a sharp pain underneath your diaphragm. (Very, very true! It’s strange how the pain presents itself in these locations — so don’t be surprised when you’re wondering why places that weren’t involved in the surgery start hurting.)
The carbon dioxide that remains in your body after the surgery may present itself as shoulder pain or a sharp pain underneath your diaphragm. (Very, very true! It’s strange how the pain presents itself in these locations — so don’t be surprised when you’re wondering why places that weren’t involved in the surgery start hurting.)
![]() Your feet are in stirrups at least part of the time, which could result in some lower back pain after the surgery from all the poking and prodding. (I only felt a small amount of lower back pain afterwards.)
Your feet are in stirrups at least part of the time, which could result in some lower back pain after the surgery from all the poking and prodding. (I only felt a small amount of lower back pain afterwards.)
![]() The pain medicine will mask your pain — to help you feel better. Agreed, the Percocet (oxycodone) lessened the pain, but it still wasn’t easy to forget about the uncomfortableness. In fact, I think it only lessened the pain due to the fact that Percocet was like a sleeping pill for me. I only took the pills for one full day after surgery — every 4 hours, and after that the pain was completely tolerable. At that point, it was simply the act of twisting my stomach when getting up or turning around that moved the stitches themselves and hurt the most. On a scale of 1 to 10, the worst pain I ever felt (with pain meds or without) would rate as a 6. They say to take 1 to 2 pills every 4 to 6 hrs. I took 1 every 4 hours.
The pain medicine will mask your pain — to help you feel better. Agreed, the Percocet (oxycodone) lessened the pain, but it still wasn’t easy to forget about the uncomfortableness. In fact, I think it only lessened the pain due to the fact that Percocet was like a sleeping pill for me. I only took the pills for one full day after surgery — every 4 hours, and after that the pain was completely tolerable. At that point, it was simply the act of twisting my stomach when getting up or turning around that moved the stitches themselves and hurt the most. On a scale of 1 to 10, the worst pain I ever felt (with pain meds or without) would rate as a 6. They say to take 1 to 2 pills every 4 to 6 hrs. I took 1 every 4 hours.
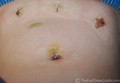
![]() You will have a 1/2-inch incision at the lower part of your navel, with stitches that will dissolve. You will have 2 to 4 tiny (1/4-inch) incisions near the pubic hair line. These incisions accommodate the instruments needed to perform endometriosis surgery. They may or may not have stitches under the bandages. (Mine did… and they took forever to fall out or disintegrate or whatever they do. For me, the healing time for those 3 prong marks took nearly 2 months to completely go away.) UPDATE: Today, 9 years later, I have absolutely no scars from my endometriosis surgery. It took about a year or so for the initial (very minor) incision scars to completely disappear.
You will have a 1/2-inch incision at the lower part of your navel, with stitches that will dissolve. You will have 2 to 4 tiny (1/4-inch) incisions near the pubic hair line. These incisions accommodate the instruments needed to perform endometriosis surgery. They may or may not have stitches under the bandages. (Mine did… and they took forever to fall out or disintegrate or whatever they do. For me, the healing time for those 3 prong marks took nearly 2 months to completely go away.) UPDATE: Today, 9 years later, I have absolutely no scars from my endometriosis surgery. It took about a year or so for the initial (very minor) incision scars to completely disappear.

![]() You can remove the waterproof bandages 2 days after surgery. (I took one quick peek, and then decided to put them right back on. I didn’t want to take any chances with those butterfly stitches & crusty spots. Not even a “regular” bandage would’ve worked, in my opinion — especially not over the belly button itself, which was far worse than the prong wounds. So I just showered with them on for about 4 days longer than required.)
You can remove the waterproof bandages 2 days after surgery. (I took one quick peek, and then decided to put them right back on. I didn’t want to take any chances with those butterfly stitches & crusty spots. Not even a “regular” bandage would’ve worked, in my opinion — especially not over the belly button itself, which was far worse than the prong wounds. So I just showered with them on for about 4 days longer than required.)
![]() You can eat normally immediately after surgery. (Not that you’ll actually want to, but it’s A-ok to. I got home from surgery at 11AM and by 7PM I felt that my stomach could handle a couple slices of pizza and a fruit smoothie. I had no problems.)
You can eat normally immediately after surgery. (Not that you’ll actually want to, but it’s A-ok to. I got home from surgery at 11AM and by 7PM I felt that my stomach could handle a couple slices of pizza and a fruit smoothie. I had no problems.)

![]() You can pretty much do whatever you’re used to doing the day after endometriosis surgery. I remember thinking it was odd that I was sitting cross-legged on my bed without any pain to speak of within hours of the surgery, yet 3 days later I was unable to stand upright without wincing in pain from my ribcage. In my case, this was due to the fact that I wasn’t able to have a bowel movement (see below).
You can pretty much do whatever you’re used to doing the day after endometriosis surgery. I remember thinking it was odd that I was sitting cross-legged on my bed without any pain to speak of within hours of the surgery, yet 3 days later I was unable to stand upright without wincing in pain from my ribcage. In my case, this was due to the fact that I wasn’t able to have a bowel movement (see below).
The Things They Forget To Mention (…to me, anyway!)
![]() They won’t perform the surgery if you have a fever on the morning of surgery. (I was paranoid that I was going to come down with a cold or something!)
They won’t perform the surgery if you have a fever on the morning of surgery. (I was paranoid that I was going to come down with a cold or something!)
![]() The week prior to your surgery, you have to have bloodwork done (at the lab of the surgery center itself), and get an EKG if you’re over 40 (at the outpatient area of the hospital adjoining the surgery center). That is, unless you’ve had these done within 2 months of your surgery date. (The whole process took about an hour for me — though each procedure itself takes less than 5 minutes apiece.)
The week prior to your surgery, you have to have bloodwork done (at the lab of the surgery center itself), and get an EKG if you’re over 40 (at the outpatient area of the hospital adjoining the surgery center). That is, unless you’ve had these done within 2 months of your surgery date. (The whole process took about an hour for me — though each procedure itself takes less than 5 minutes apiece.)
![]() The EKG is not as bad as it sounds. You’re fully clothed, and they simply put some sticky tabs on your legs, your chest, your back, and your arms. You lie quietly for about 30 seconds, and the machine measures your heart rate & breathing patterns. It’s not the same as an Echocardiogram — I had one of those before (specifically, a TTE).
The EKG is not as bad as it sounds. You’re fully clothed, and they simply put some sticky tabs on your legs, your chest, your back, and your arms. You lie quietly for about 30 seconds, and the machine measures your heart rate & breathing patterns. It’s not the same as an Echocardiogram — I had one of those before (specifically, a TTE).

![]() You can’t wear any of your own metal into surgery, but you can wear plenty of theirs. Not only did one of my wristbands that identified my blood type have a full metal clasp, but when I got home, I found a heart-monitor plug still attached to the back left side of my chest area — it was one of those with a metal node. (TIP: Goo Gone makes removing them a cinch!)
You can’t wear any of your own metal into surgery, but you can wear plenty of theirs. Not only did one of my wristbands that identified my blood type have a full metal clasp, but when I got home, I found a heart-monitor plug still attached to the back left side of my chest area — it was one of those with a metal node. (TIP: Goo Gone makes removing them a cinch!)
![]() Before you change into your cap & gown, you have to pee in a cup for a last-minute pregnancy test.
Before you change into your cap & gown, you have to pee in a cup for a last-minute pregnancy test.
![]() You have to wear these fairly tight knee-high socks that are cut-out at the toe part. They’re to prevent blood clots in your legs. (Not sure why they’re cut-out at the toe …So they can play “this little piggy” when they’re trying to get you to come around in recovery???)
You have to wear these fairly tight knee-high socks that are cut-out at the toe part. They’re to prevent blood clots in your legs. (Not sure why they’re cut-out at the toe …So they can play “this little piggy” when they’re trying to get you to come around in recovery???)
![]() On top of those socks, you have to put on their fun little socks with grippies on the bottom — so you don’t slip if you walk on their uncarpeted floors. (I love these… I actually took mine home and wear them around the house all the time… they’re GREAT!)
On top of those socks, you have to put on their fun little socks with grippies on the bottom — so you don’t slip if you walk on their uncarpeted floors. (I love these… I actually took mine home and wear them around the house all the time… they’re GREAT!)
![]() Not sure why the “grippies” on the socks were required, because I didn’t have to walk anywhere. They pushed me on a gurney from pre-op to the surgery room & vice versa. And I even got a free ride in a wheelchair out to the car. (I remember telling the recovery nurse how good it felt for a Type A personality who’s always in control of things to spend the past couple of hours completely being taken care of for a change.)
Not sure why the “grippies” on the socks were required, because I didn’t have to walk anywhere. They pushed me on a gurney from pre-op to the surgery room & vice versa. And I even got a free ride in a wheelchair out to the car. (I remember telling the recovery nurse how good it felt for a Type A personality who’s always in control of things to spend the past couple of hours completely being taken care of for a change.)
![]() You have to be intubated / have a tracheotomy. This terrified me the moment I heard the nurse slip-up and mention this in pre-op. But it’s really not so bad — because you’re asleep when they do it. Once I knew I’d be asleep, I was fine. (But it certainly didn’t help that the night before I’d watched some doctor show where they couldn’t get the trach tube down a guy’s throat — for some reason, he was awake throughout the process, which would make it much more difficult.)
You have to be intubated / have a tracheotomy. This terrified me the moment I heard the nurse slip-up and mention this in pre-op. But it’s really not so bad — because you’re asleep when they do it. Once I knew I’d be asleep, I was fine. (But it certainly didn’t help that the night before I’d watched some doctor show where they couldn’t get the trach tube down a guy’s throat — for some reason, he was awake throughout the process, which would make it much more difficult.)

![]() They “catheterize” you. But, just like the trach tube… you’re completely asleep & won’t remember a thing about it. (Good news: There’s no lasting evidence, nor any pain at all after you’ve had a catheter removed.)
They “catheterize” you. But, just like the trach tube… you’re completely asleep & won’t remember a thing about it. (Good news: There’s no lasting evidence, nor any pain at all after you’ve had a catheter removed.)
![]() They tape your eyes shut during surgery. How I found this out: The morning after, my left eyelid kept sticking to itself. This was the point at which I discovered tape residue underneath both eyes.
They tape your eyes shut during surgery. How I found this out: The morning after, my left eyelid kept sticking to itself. This was the point at which I discovered tape residue underneath both eyes.
![]() For outpatient surgeries (at least at the hospital I went to), the surgery room itself is more or less just a big open cafeteria-like room filled with people on gurneys — separated by individual curtains. I was surprised that it didn’t look more sterile and private. But then again, we were all there for some pretty routine stuff in the outpatient surgery center.
For outpatient surgeries (at least at the hospital I went to), the surgery room itself is more or less just a big open cafeteria-like room filled with people on gurneys — separated by individual curtains. I was surprised that it didn’t look more sterile and private. But then again, we were all there for some pretty routine stuff in the outpatient surgery center.
![]() As soon as you come to and can carry on a conversation with the recovery nurse, you’re given a Percocet. They have to wait 10 minutes to see how your body reacts, then they give you a Saltine cracker and your choice of beverage — to make sure you can hold down food before you leave. (When I told her I was still feeling the pain pretty good at the belly button region, she gave me another Percocet and we waited another 10 minutes. As a result, I was feeling perfectly fine & painless for the rest of the day. In fact, Jim was amazed I was able to dress myself and even bend down to tie my own shoes. I guess I was kind of in la-la-land.)
As soon as you come to and can carry on a conversation with the recovery nurse, you’re given a Percocet. They have to wait 10 minutes to see how your body reacts, then they give you a Saltine cracker and your choice of beverage — to make sure you can hold down food before you leave. (When I told her I was still feeling the pain pretty good at the belly button region, she gave me another Percocet and we waited another 10 minutes. As a result, I was feeling perfectly fine & painless for the rest of the day. In fact, Jim was amazed I was able to dress myself and even bend down to tie my own shoes. I guess I was kind of in la-la-land.)
![]() You may become constipated afterwards, which could wreak havoc on your healing process — so be sure to start with some stool softeners after the first day at home. I didn’t start this until the 3rd day after endometriosis surgery — which meant I endured too many days of sharp poking pains anytime I’d breathe in. (They said it was something about my innards poking my ribs or lungs or something. The result was much, much pain!)
You may become constipated afterwards, which could wreak havoc on your healing process — so be sure to start with some stool softeners after the first day at home. I didn’t start this until the 3rd day after endometriosis surgery — which meant I endured too many days of sharp poking pains anytime I’d breathe in. (They said it was something about my innards poking my ribs or lungs or something. The result was much, much pain!)
![]() At one point, the pain was so severe, I wondered if I was having an appendicitis attack or something. I couldn’t move without making the pain worse. That’s when I called my doctor and was told that I needed to have my first B.M. immediately! She recommended Colace stool softener and if the pain continued to go to the emergency room. That day, nothing changed. The next morning, I was about to head to the emergency room, when I decided to try eating some oatmeal first instead. Fortunately, that was enough to trigger the goodness. From that point forward, the sharp pains began to subside and I was able to stand up straight for the very first time in days. (TIP: Don’t purchase a stool softener that has a laxative in it. If Colace is not available, Dulcolax will work just the same.)
At one point, the pain was so severe, I wondered if I was having an appendicitis attack or something. I couldn’t move without making the pain worse. That’s when I called my doctor and was told that I needed to have my first B.M. immediately! She recommended Colace stool softener and if the pain continued to go to the emergency room. That day, nothing changed. The next morning, I was about to head to the emergency room, when I decided to try eating some oatmeal first instead. Fortunately, that was enough to trigger the goodness. From that point forward, the sharp pains began to subside and I was able to stand up straight for the very first time in days. (TIP: Don’t purchase a stool softener that has a laxative in it. If Colace is not available, Dulcolax will work just the same.)
![]() I’ve read that you can resume sexual activity after 2 to 3 days (which, quite honestly, I couldn’t imagine being very enjoyable), but my doctor said to wait 2 weeks. This might have had something to do with the size of my cysts — baseball-sized on one ovary, golf ball size on the other.
I’ve read that you can resume sexual activity after 2 to 3 days (which, quite honestly, I couldn’t imagine being very enjoyable), but my doctor said to wait 2 weeks. This might have had something to do with the size of my cysts — baseball-sized on one ovary, golf ball size on the other.

![]() Your throat will be a tad sore for 2 to 3 days afterwards from the trach tube. It’s not unbearable, just noticeable. And your voice sounds slightly higher pitched for a couple days too.
Your throat will be a tad sore for 2 to 3 days afterwards from the trach tube. It’s not unbearable, just noticeable. And your voice sounds slightly higher pitched for a couple days too.
![]() If you have crowns on any of your front teeth, they need to know about it. (I had to sign a release acknowledging that there could be “dental damage” from the intubation process itself. They said it could occur if you have crowns in front.)
If you have crowns on any of your front teeth, they need to know about it. (I had to sign a release acknowledging that there could be “dental damage” from the intubation process itself. They said it could occur if you have crowns in front.)
![]() Afterwards, you may have cuts on your lip that swell up whenever you eat hot soup other warm foods & beverages. (I presume this is from the intubation process and/or one of the crowns I had on a front tooth.) A spot on my top lip swelled up for over a week after the surgery — only whenever I ate something hot or cold.
Afterwards, you may have cuts on your lip that swell up whenever you eat hot soup other warm foods & beverages. (I presume this is from the intubation process and/or one of the crowns I had on a front tooth.) A spot on my top lip swelled up for over a week after the surgery — only whenever I ate something hot or cold.
![]() When you’re feeling those pains in your shoulders, neck, back, and chest from the excess air, it helps to get up and move around. It’s also a good idea to drink either hot water or hot tea with fresh lemon. A heating pad will help too.
When you’re feeling those pains in your shoulders, neck, back, and chest from the excess air, it helps to get up and move around. It’s also a good idea to drink either hot water or hot tea with fresh lemon. A heating pad will help too.

![]() The intense pains you feel after surgery can jump from one side to the other, with no rhyme or reason. For instance, the cyst on my left side was the largest, yet that was the side that hurt the least overall. The right side would often hurt so badly I’d double-over to get through the pain. Only to find, that an hour or so later, a similarly intense pain was occurring on the left side this time.
The intense pains you feel after surgery can jump from one side to the other, with no rhyme or reason. For instance, the cyst on my left side was the largest, yet that was the side that hurt the least overall. The right side would often hurt so badly I’d double-over to get through the pain. Only to find, that an hour or so later, a similarly intense pain was occurring on the left side this time.
![]() You will return to your doctor’s office for a post-op checkup about 2 weeks after surgery. At that appointment, your doctor will discuss the results of your endometriosis surgery and answer any further questions you may have.
You will return to your doctor’s office for a post-op checkup about 2 weeks after surgery. At that appointment, your doctor will discuss the results of your endometriosis surgery and answer any further questions you may have.
![]() You’ll probably lose some weight. According to my doctor, I lost 15 pounds! (While the weight loss after laparoscopy is largely due to the fact that you’re eating less while recuperating, I also attribute my lost weight to the removal of a baseball and a golf ball from inside me!)
You’ll probably lose some weight. According to my doctor, I lost 15 pounds! (While the weight loss after laparoscopy is largely due to the fact that you’re eating less while recuperating, I also attribute my lost weight to the removal of a baseball and a golf ball from inside me!)
How I Learned I Had Severe Endometriosis
 I wasn’t really having any endometriosis symptoms at the time that I was diagnosed with severe endometriosis. I simply went to the gynecologist one day after a 2 to 3 year span of not having been to one.
I wasn’t really having any endometriosis symptoms at the time that I was diagnosed with severe endometriosis. I simply went to the gynecologist one day after a 2 to 3 year span of not having been to one.
When we talked about how I hadn’t been able to get pregnant the past 6 years… and about my heavy periods… and about ONE night several months ago that unexplainedly left me doubled over in pain and ready to call an ambulance… she thought we should do a trans-vaginal ultrasound — just for the heck of it, more as a precaution than anything else.
When the ultrasound revealed a cyst on both the left and right ovaries, my first thought was to just “live with it”.
Why? Because I knew that cysts on ovaries are actually quite common. And they are usually associated with pure ‘ol endometriosis — a sometimes painful, yet common condition that you can live with.
What scared me most were the stories I’d heard. For example, most people say that even if you remove the endometriosis, it’s practically a given that the endometriosis will reappear again and again in the future.
And since my endometriosis symptoms weren’t really that bad — in my mind — I feared that I’d actually be triggering more symptoms and more pain and more endometriosis. In the end, we chose the most aggressive form of treatment in order to get to the root of the problem… fast.
While the cysts were larger than everyone initially thought, they were not cancerous. (Thank goodness.)
And the bonus from my endometriosis surgery — the optional ablation — meant no more periods. Ever!
Truthfully, I wasn’t initially going to do the ablation. But when the doctor said she would actually like to have this option herself — and my hubby mentioned that I would probably be happier if I did it — I realized that it was probably a good idea. Now I can say I’m very glad I did it. It’s one of the best things I’ve ever done.
Endometriosis No More?
 For the record, this laparoscopy or surgery isn’t really a an endometriosis cure — it’s just a temporary fix because endometriosis tends to show itself again.
For the record, this laparoscopy or surgery isn’t really a an endometriosis cure — it’s just a temporary fix because endometriosis tends to show itself again.
The good part is you can do things to keep endometriosis from recurring so aggressively like:
- Take birth control pills — I’ve been taking , a very low-dose birth control pill since the surgery.
- Treat it differently the next time it occurs — Now that I know any future bouts of endometriosi probably won’t be cancerous in my case, I could treat recurrences with those shots I talked about earlier.
Another interesting fact: By its very nature, I guess endometriosis sort of invades your body and latches onto your linings all throughout your body. For example, they think endometriosis could be the explanation for some weird chest pains I’ve had for years (actually decades). Doesn’t make sense to me, but that’s what my other (family practice) doctor told me.
So… once you have endometriosis, you always have endometriosis. But you can totally live with it. It’s not life-threatening in any way (unless yours is cancerous). The only difference is the degree of pain that different people have from it. I had next to none.
For More Information About Endometriosis Surgery…
- What to expect after your laparoscopy – a more detailed summary of the things I’ve stated above.
- Laparoscopy before & after tips – an overview of what you can expect.
- Endometriosis slideshow – what it’s like… in pictures.
- 10 tips for a successful endometriosis laparoscopy recovery – helpful tips for the healing process.
- What endometriosis looks like – a video of the laparoscopic procedure.
- How to prepare for your laparoscopy – from a person who’s had 3 of them!
- Endometriosis Multimedia Gallery – photos and videos showing endometriosis at its finest.
And now for the humor…
About a week after my endometriosis surgery, comedians Bob & Tom talked about this exact thing! Actually, they were talking more about the ultrasound that’s required to initially identify things like cysts… and endometriosis… and even a tilted uterus. (Yep, I happen to have one of those, too.)
Audio clip from the Nov. 15, 2006 Bob & Tom Show where they talked about Christy’s tilted uterus.
Audio clip from the Nov. 16, 2006 Bob & Tom Show where they played the song “Tilted Uterus” by Duke Tomato.
See… if you look hard enough, you can find humor in just about anything!
My Endometriosis Returned, So I Had A Hysterectomy
Just 9 years after my endometriosis surgery, I was starting to have some weird internal pains on occasion.
While I didn’t have any other signs of endometriosis, my doctor suggested I have another transvaginal ultrasound just to be sure.
Yep, the endometriosis returned… and quite aggressively (again)!
Where most women’s ovaries float freely to the sides, mine were firmly attached to the back side of my uterus — due to the severe endometriosis.
For me, the only signs that the endometriosis might be returning were: painful sex and highly unusual spotting (since I don’t normally have periods — or spotting — due to the endometrial ablation mentioned above).
Pain with intercourse can occur from fibroids at the front or top of the uterus. This is an unusual symptom, but it can occur. Source
Fibroids are noncancerous growths that originate from the muscle of the womb (or uterus). They affect 80% of all women, and some patients suffer from heavy bleeding & pain. Source
My 2 endometriosis treatment options:
- I could opt for a medical treatment to hopefully keep the endometriosis at bay (a 6-month course of Lupron shots) — which would trick my body into menopause temporarily.
- Or I could opt for a full hysterectomy.
I chose the full hysterectomy since I was almost 50 and the Lupron would basically just serve as a “bandaid” requiring regular tests and more medication until I reached menopause.
My regular gynecologist immediately sent me to a gynecological cancer specialist who uses the DaVinci robotic surgery method for hysterectomies here in Nashville, TN. My full hysterectomy was scheduled right away.
Here’s a summary of my experience: What It’s Like To Have A Hysterectomy Surgery & What My Recovery Was Like
And if you’re planning to have a hysterectomy soon, here are my best tips: Before You Have A Hysterectomy, Read These Tips That Helped Me Prepare For My Full Hysterectomy
So now the question is… can you still have endometriosis after hysterectomy? My doctors both told me YES. So we’ll see what’s in the cards for me…





